*Małgorzata Kołodziejczak1, 2, Przemysław Ciesielski1, 2
When to perform anoplasty – our clinical experience and current research
Kiedy wykonywać anoplastykę – doświadczenia własne i aktualne doniesienia
1Warsaw Proctology Center, St. Elizabeth’s Hospital in Warsaw
2Department of General Surgery, District Hospital in Ostrów Mazowiecka
Streszczenie
Pierwsze operacje plastyczne kanału odbytu przeprowadzane były u dzieci z powodu wrodzonych wad odbytu, a historia wykonywania tych zabiegów sięga XIX wieku. Operacje plastyczne odbytu, pomijając wady rozwojowe u dzieci, najczęściej są wykonywane z powodu powikłań po przeprowadzanych na odbycie zabiegach chirurgicznych. W artykule omówiono najczęściej wykonywane zabiegi plastyczne w kanale odbytu, przedstawiając je na tle jednostek chorobowych, takich jak: zwężenie odbytu, deformacja odbytu po operacjach proktologicznych związana z nieszczelnością odbytu i brudzeniem bielizny i/lub nietrzymaniem gazów i stolca, deformacje po zabiegach onkologicznych, zniekształcenia krocza po traumatycznych porodach, nawrotowa szczelina oraz defekty kosmetyczne. Prawidłowo wykonana anoplastyka może znacznie poprawić kosmetykę, funkcje czynnościowe i w konsekwencji jakość życia pacjenta. Wskazano też na pewne działania profilaktyczne, czyli zapobieganie niektórym zniekształceniom odbytu, co np. w przypadku zwężeń odbytu wiąże się nie tylko z prawidłową techniką operacyjną, ale i z kontrolami po operacji, np. w przypadku fistulotomii z zastosowaniem techniki FIPS. Pacjent kwalifikowany do anoplastyki powinien być operowany przez doświadczony zespół chirurgów w ośrodku referencyjnym. Zwiększa to wówczas jego szanse na pełny powrót do zdrowia.
Summary
First plastic repairs of the anal canal, which date back to the 19th century, were performed in children with congenital anal malformations. In addition to developmental malformations in children, anal reconstructions are most often performed due to postoperative complications. The paper discusses the most common anal canal plasty procedures performed for anal stenosis, anal deformation secondary to proctological surgeries resulting in anal leakage and underwear staining and/or gas and faecal incontinence, deformities after oncological procedures, childbirth-related perineal deformities, as well as recurrent anal fissure and cosmetic defects. Properly performed anoplasty can significantly improve cosmetic and functional outcomes, which translates into higher quality of life. It has also been suggested to implement certain prophylactic measures to avoid some anal deformities, which, for example, in the case of anal stenosis, involves only a correct surgical technique, but also postoperative follow-up, e.g. in the case of fistulectomy and fistulectomy and primary sphincteroplasty (FIPS). Anoplasty should be performed by an experienced team of surgeons in a reference centre. This increases the chances for a full recovery.
Słowa kluczowe: anoplastyka, FIPS, deformacja typu dziurki od klucza

Introduction
The first plastic repairs of the anal canal were performed in children due to congenital malformations of the anus. These procedures date back to the 19th century, when in 1835 a French surgeon Jean Amussat treated congenital anal atresia with an anastomosis of the rectal wall with perineal stomy. Alberto Peña, the head of the Department of Surgery in Mexico, who introduced posterior sagittal anorectoplasty, was a pioneer in anoplasty. Interestingly, this surgeon questioned the existence of the puborectalis muscle, pointing to the funnel-shaped muscle fibres as the sphincter mechanism. Apart from developmental malformations in children, anal reconstructions are most often performed due to postoperative complications. In addition to congenital anorectal malformations in children, indications for anal canal plasty in patients of all ages include:
– anal stenosis,
– postoperative anal deformity leading to anal leakage and underwear staining and/or gas and faecal incontinence,
– perineal deformity after traumatic childbirth,
– recurrent anal fissure,
– cosmetic defects: postoperative scarring, hypertrophied anodermal folds,
– reconstruction of an extensive defect in anal circumference due to excision of tumours or precancerous lesions.
Surgical approaches
The choice of surgical technique depends on the reason for patient qualification for surgery. The most commonly used anoplasty methods include:
– simple excision of the deforming scar with or without suturing the internal sphincter and the subcutaneous part of the external sphincter, with the anoderm sutured over the muscles,
– excision of the scar and closing the anal canal defect with a house flap, a rhomboid flap, or a Y-V flap.
– excision of hypertrophied anodermal folds and skin overhangs with radial incisions in relation to the anal canal.
Anal stenosis
Anal stenosis usually develops as a complication after anorectal procedures, most often after haemorrhoidectomy (fig. 1). This may be due to excessively extensive excision of the anoderm without leaving healthy tissue bridges of adequate width (minimum 5 mm) between the wounds in the anal canal. Anal canal stenosis may also be associated with ongoing chronic inflammation as a complication of poor postoperative healing or as a result of inflammatory bowel disease (Crohn’s disease, ulcerative colitis), past radiotherapy and anal canal trauma. Milsom and Mazier classification distinguishing mild, moderate and severe anal stenosis, is a commonly used grading system. Classification based on the degree of stenosis, which distinguishes low (at least 0.5 cm below the dentate line), medium (0.5 cm proximal to 0.5 cm distal to the dentate line), and high stenosis (proximal to 0.5 cm above the dentate line), is practical from the surgeon’s point of view.
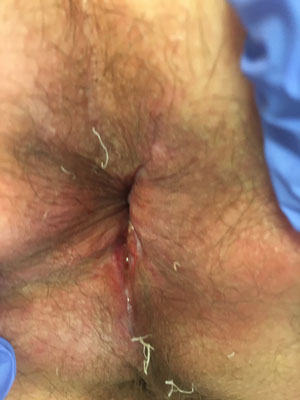
Fig. 1. Anal stenosis
Prevention of postoperative stenosis is based on proper surgical technique as well as thorough postoperative follow-up and proper patient education on anal dilation in the period between follow-up visits.
Conservative treatment
Conservative methods, including a high-fibre diet, adequate hydration, dietary fibre and bulk-forming laxatives, as well as mechanical dilatation, digital anal dilation or the use of special dilators, are always used as the first-line treatment for anal stenosis.
It should be mentioned that there is still an ongoing discussion on the role of mechanical dilation in the treatment of anal strictures (1). In the case of worsening clinical symptoms and grade III stenosis (impossible insertion of the little finger), the patient should be qualified for surgical treatment (1).
Surgical treatment
Excision of the stenotic scar is the simplest procedure. However, the effect is usually short-term as another scar is formed after a few months, and the stenosis recurs. Therefore, an anodermal flap is usually placed at the site of the excised scar, whereas a rectal mucosal flap can be used in the case of higher stenoses. In our practice, however, we most often use an anodermal flap. When forming an advancement flap, naturally hypertrophied anodermal folds can be used or an anodermal flap of various shapes can be recruited.
Anal stenosis is an uncommon condition and the available reports are based on small groups of patients (2).
An interesting study in a group of 11 patients with anal stenosis was presented by Duieb et al. (2). Patients were assessed for symptoms, cause of anal stenosis, type of anoplasty, complications and treatment efficacy. All procedures were performed by the same surgeon in three hospitals.
Previous surgeries, tumours and anal fissures were the main aetiological factors of stenosis in the study group. Transverse suturing and Y-V or diamond-shaped flaps were used. No significant postoperative complications were observed. The authors of the paper concluded that anoplasty is a safe and effective therapeutic option for anal stenosis.
One of the recent (2022) meta-analyses assessed 29 studies in 556 patients. Anal stenosis developed as a complication after haemorrhoidectomy in 3/4 of cases. Y-V flap anoplasty was the most common procedure (29%). The best treatment outcomes in terms of clinical symptom remission and improvement of the quality of life were obtained in patients after anoplasty with house advancement flap.
Powyżej zamieściliśmy fragment artykułu, do którego możesz uzyskać pełny dostęp.
Mam kod dostępu
- Aby uzyskać płatny dostęp do pełnej treści powyższego artykułu albo wszystkich artykułów (w zależności od wybranej opcji), należy wprowadzić kod.
- Wprowadzając kod, akceptują Państwo treść Regulaminu oraz potwierdzają zapoznanie się z nim.
- Aby kupić kod proszę skorzystać z jednej z poniższych opcji.
Opcja #1
29 zł
Wybieram
- dostęp do tego artykułu
- dostęp na 7 dni
uzyskany kod musi być wprowadzony na stronie artykułu, do którego został wykupiony
Opcja #2
69 zł
Wybieram
- dostęp do tego i pozostałych ponad 7000 artykułów
- dostęp na 30 dni
- najpopularniejsza opcja
Opcja #3
129 zł
Wybieram
- dostęp do tego i pozostałych ponad 7000 artykułów
- dostęp na 90 dni
- oszczędzasz 78 zł
Piśmiennictwo
1. Chiarelli M, Guttadauro A, Maternini M et al.: The clinical and therapeutic approach to anal stenosis. Review Ann Ital Chir 2018; 89: 237-241.
2. Duieb Z, Appu S, Hung K, Nguyen H: Anal stenosis: use of an algorithm to provide a tension-free anoplasty. ANZ J Surg 2010; 80(5): 337-340.
3. Parkash S, Lakshmiratan V, Gajendran V: Fistula-in-ano: treatment by fistulectomy, primary closure and reconstitution. Aust N Z J Surg 1985; 55: 23-27.
4. Ji L, Zhang Y, Xu L et al.: Advances in the Treatment of Anal Fistula: A Mini-Review of Recent Five-Year Clinical Studies. Front Surg 2021; 7: 586891.
5. De Hous N, Van den Broeck T, de Gheldere C: Fistulectomy and primary sphincteroplasty (FIPS) to prevent keyhole deformity in simple anal fistula: a single-center retrospective cohort study. Acta Chir Belg 2021; 121(5): 308-313.
6. Aguilar-Martínez MDM, Sánchez-Guillèn L, Barber-Valles X et al.: Long-term Evaluation of Fistulotomy and Immediate Sphincteroplasty as a Treatment for Complex Anal Fistula. Dis Colon Rectum 2021; 64(11): 1374-1384.
7. Litta F, Parello A, De Simone V et al.: Fistulotomy and primary sphincteroplasty for anal fistula: long-term data on continence and patient satisfaction. Tech Coloproctol 2019; 23(10): 993-1001.
8. Farid M, Youssef M, El Nakeeb A et al.: Comparative study of the house advancement flap, rhomboid flap, and Y-V anoplasty in treatment of anal stenosis: a prospective randomized study. Dis Colon Rectum 2010; 53(5): 790-797.
9. Sentovich SM, Falk PM, Christensen MA et al.: Operative results of House advancement anoplasty. Br J Surg 1996; 83(9): 1242-1244.
10. Alver O, Ersoy YE, Aydemir I et al.: Use of „house” advancement flap in anorectal diseases. World J Surg 2008; 32(10): 2281-2286.
11. Kołodziejczak M, Ciesielski P, Kucharczyk A: Standardy leczenia szczeliny odbytu w Europie i w Stanach Zjednoczonych. Nowa Med 2021; 28(2): 80-88.
12. D’Orazio B, Cudia B, Bonventre S et al.: Fissurectomy and anoplasty in posterior normotensive chronic anal fissure. Acta Biomed 2021; 92(5): e2021176.
13. Sahebally SM, Walsh SR, Mahmood W et al.: Anal advancement flap versus lateral internal sphincterotomy for chronic anal fissure – a systematic review and meta-analysis. Int J Surg 2018; 49: 16-21.
14. Gallo G, Picciariello A, Di Tanna GL et al.: Anoplasty for anatomical anal stenosis: systematic review of complications and recurrences. Colorectal Dis 2022; 24(12): 1462-1471.
15. D’Orazio B, Geraci G, Martorana G et al.: Fisurectomy and anoplasty with botulinum toxin injection in patients with chronic anal posterior fissure with hypertonia: a long-term evaluation. Updates Surg 2021; 73(4): 1575-1581.

